Get Ready for the San Diego Rock ‘n’ Roll Marathon
The San Diego Rock ‘n’ Roll marathon is coming up! You are likely finishing your build phases of training and are headed into a much needed taper to help rebuild your body before the big day. Now that training volume has decreased, you have more time to address your body to get it into tip top shape before race day. Beyond foam rolling, stretching, and mobility work, the following are services that can help decrease tightness, soreness, aches, and pains before your big day. Our office accepts most major insurances and offers affordable cash rates. Our San Diego Chiropractors treat runners and running injuries on a daily basis using the following techniques:
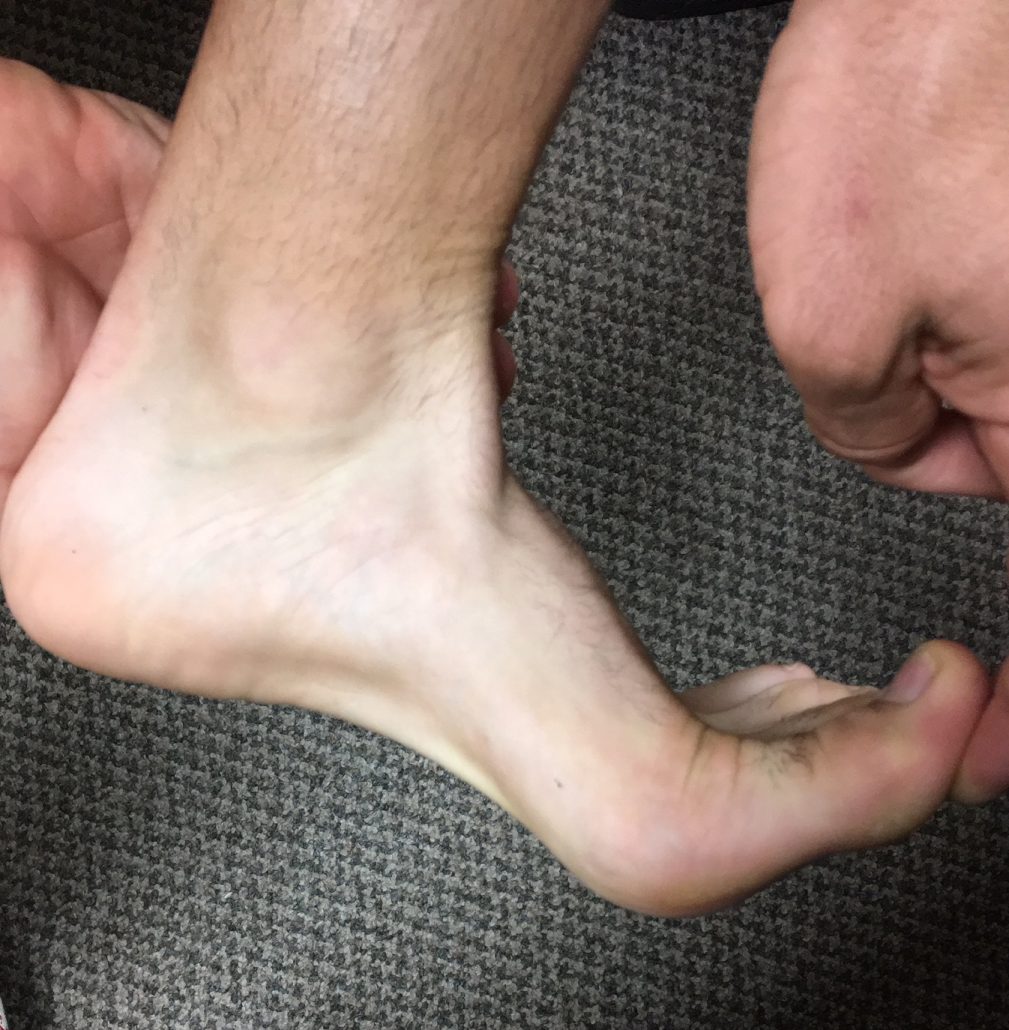
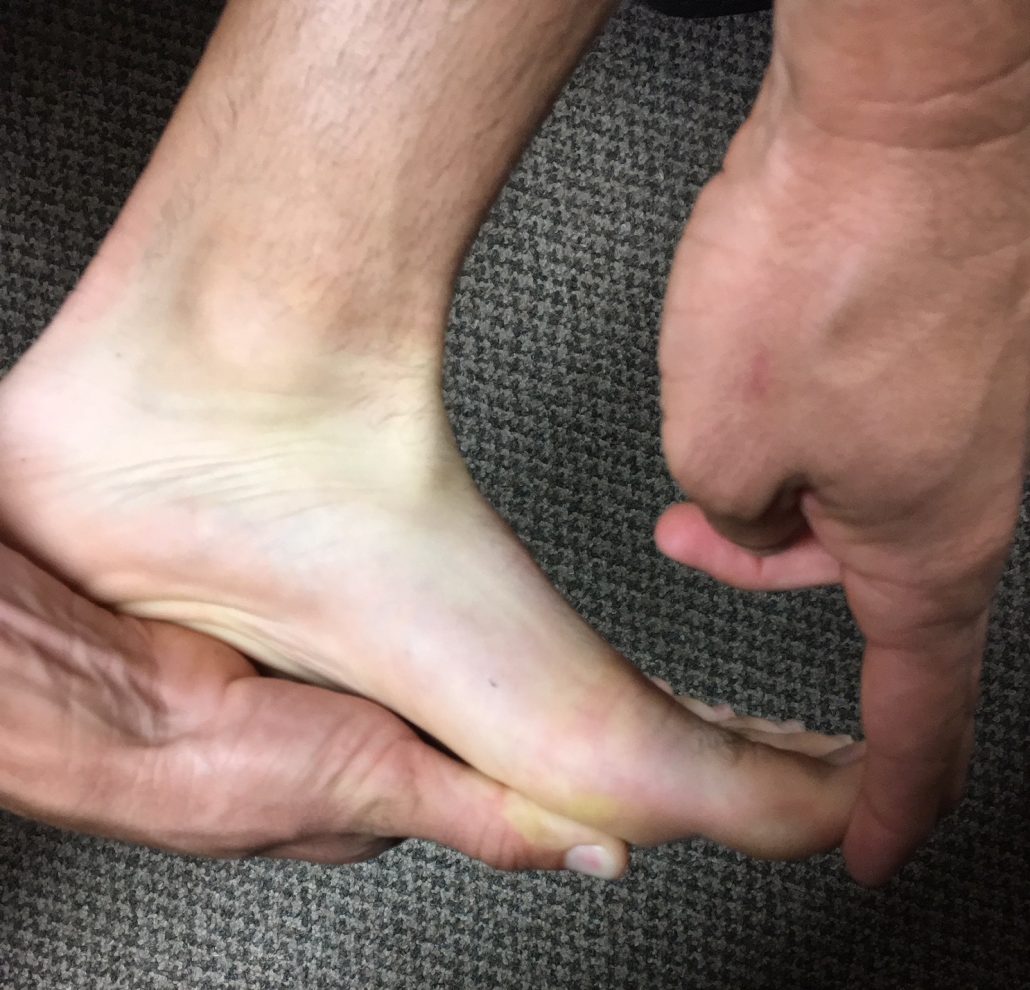
Active Release Technique– Our staff is trained in Active Release Technique which is a state of the art soft tissue injury management system. Our chiropractors utilize ART to help reduce tightness and soreness at isolated parts of the body. For example, many runners feel tight in their hips and quadriceps following long runs. One or two ART sessions before the Rock ‘n’ Roll Marathon can help rid the muscles of that tightness.

Graston Technique– While training for the Rock ‘n’ Roll Marathon, if any injury is long standing, particularly in a tendon, Graston is excellent to get ample blood supply to that area. Our San Diego Chiropractor will sometimes have runners perform movements while using the Graston tools to help facilitate movement between the fascia and muscles. Bascially, your muscles move better so you do not feel tight and sore before your race!

Spinal Manipulation– If your back is stiff and lacks proper range of motion, spinal adjustments may be the right treatment for you. Spinal manipulation is an excellent treatment to help restore proper joint mobility. Spine stiffness is a common complaint in runners especially when training for a marathon due to the long hours of training and consistent bouncing motion into the spine.
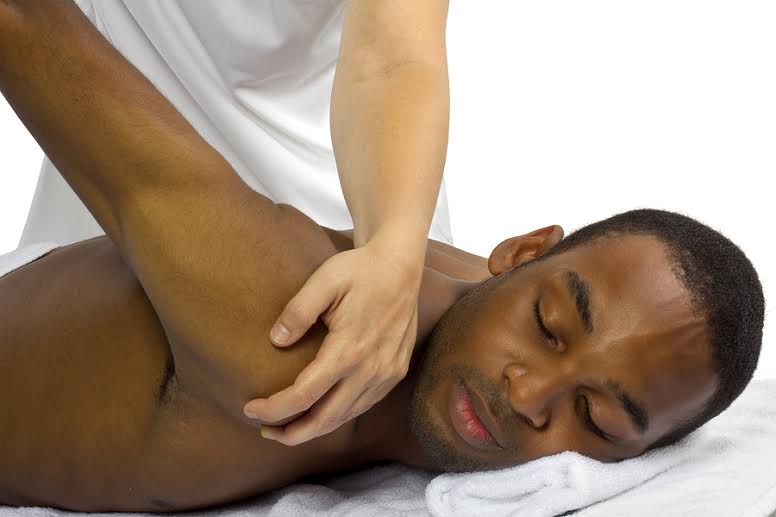
Massage Therapy– Our massage therapist is an avid runner and endurance athlete. If you have numerous areas of tightness and soreness, schedule a massage to have a nice once over to all of those complaints.
Head into your race feeling as healthy as you can and you will see great results. After the San Diego Rock ‘n’ Roll Marathon, we recommend our runners to receive treatment about once every 4 weeks to help reduce tightness in the common running muscles and joints. Our office is conveniently located in Mission Valley, San Diego near the Rock ‘n’ Roll Marathon course!
Good luck in the San Diego Rock ‘n’ Roll Marathon!